Skin Fungal Infection Pictures – Common Types and How to Spot Them
Dermatological fungal infections present characteristic visual patterns that enable preliminary identification before laboratory confirmation. These manifestations range from annular plaques with peripheral scaling to macerated interdigital webs, varying by causative organism and anatomical site.
Pathogenic fungi thrive in warm, moist microenvironments, particularly skin folds, plantar surfaces, and inguinal regions. Dermatophytes such as Trichophyton rubrum and yeast species including Candida albicans and Malassezia furfur produce erythematous, pruritic eruptions that intensify under occlusive conditions.
Transmission dynamics involve direct contact with infected keratinized tissue, asymptomatic carriers, fomites such as contaminated linens, or zoophilic reservoirs. Populations in humid climates and athletic cohorts demonstrate heightened incidence due to persistent moisture and occlusive footwear.
What Does a Skin Fungal Infection Look Like?
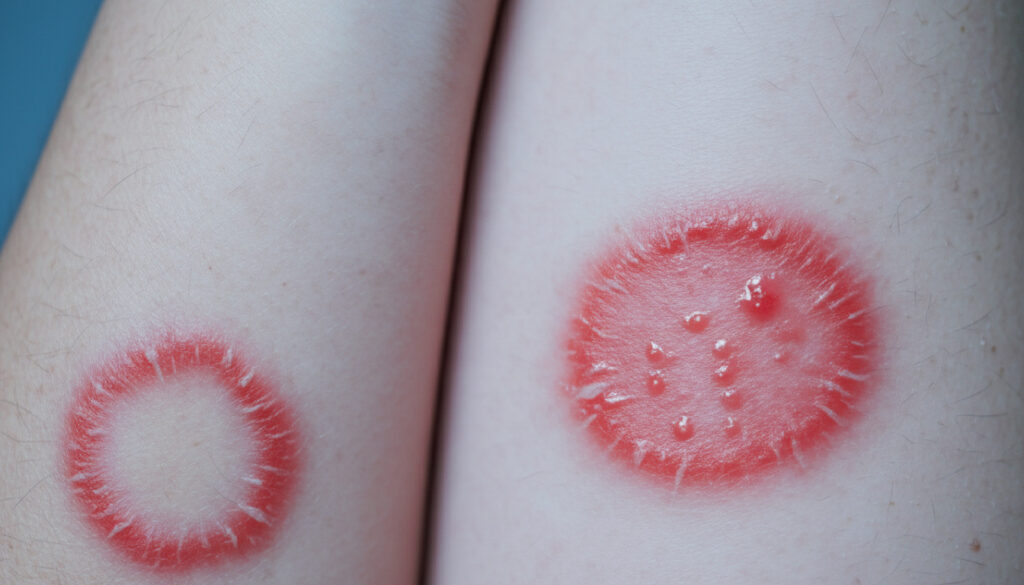
Ringworm (Tinea Corporis)
Annular erythematous plaques with raised, scaly borders and central clearing. Lesions expand centrifugally, creating distinctive ring-like configurations on trunk and extremities.
Athlete’s Foot (Tinea Pedis)
Interdigital maceration with peeling, scaling, and fissuring. Moccasin-pattern dryness affects plantar surfaces; vesicular variants present with small blisters.
Jock Itch (Tinea Cruris)
Half-moon shaped erythematous patches in groin and proximal medial thighs. Raised borders with central clearing; typically spares scrotum and penis.
Yeast Infection (Candidiasis)
Beefy-red erythema in skin folds with satellite pustules at periphery. Oozing, crusting, and maceration characterize intertriginous involvement.
- Prevalence: Dermatophyte infections affect approximately 20-25% of global population during lifetime, with tinea pedis showing highest incidence in adult males.
- Contagion period: Active lesions remain contagious until antifungal treatment initiates; Trichophyton species survive on fomites for months.
- Self-limiting vs. chronic: Untreated tinea corporis persists indefinitely; candidiasis fluctuates with moisture levels and immune status.
- OTC efficacy: Allylamines (terbinafine) demonstrate superior cure rates compared to azoles for dermatophyte infections.
- Diagnostic confirmation: Potassium hydroxide (KOH) preparation identifies hyphae with 80-90% sensitivity.
- Resistance patterns: Chronic or extensive infections require systemic therapy; topical agents fail in onychomycosis.
| Type | Visual Appearance | Common Locations | Duration Untreated |
|---|---|---|---|
| Ringworm (Tinea Corporis) | Circular lesions with scaly, raised edges; central clearing | Arms, legs, trunk, face | Months to years; progressive expansion |
| Athlete’s Foot (Tinea Pedis) | Interdigital scaling, plantar hyperkeratosis, vesicles | Toe webs, soles, lateral feet | Chronic; seasonal exacerbations |
| Jock Itch (Tinea Cruris) | Half-moon erythema with well-demarcated borders | Groin, inner thighs, buttocks | Persistent without environmental modification |
| Candida Intertrigo | Beefy-red plaques with satellite pustules | Skin folds, under breasts, groin, diaper area | Recurrent; depends on moisture control |
| Tinea Versicolor | Hypopigmented or hyperpigmented fine scaling patches | Trunk, upper arms, neck | Months; cosmetic persistence post-treatment |
| Tinea Capitis | Scaly patches with alopecia, possible kerion formation | Scalp, eyebrows, eyelashes | Requires systemic treatment; permanent alopecia possible |
Symptoms of Skin Fungal Infections
Dermatophyte-Specific Presentations
Tinea corporis produces intense pruritus accompanied by peripheral scaling. The advancing border shows active inflammation while central areas clear, creating the characteristic ring morphology. Multiple lesions may coalesce, forming gyrate patterns.
Tinea pedis manifests with stinging sensations between toes, progressing to fissuring and malodorous maceration. Hyperkeratotic variants present with diffuse moccasin-pattern scaling across plantar surfaces without significant inflammation.
Yeast Infection Characteristics
Candida species generate burning discomfort rather than pure pruritus. The presence of satellite pustules—small pustules surrounding the main erythematous plaque—distinguishes candidiasis from dermatophyte infections. Intertriginous areas under breasts and in abdominal folds show particular susceptibility.
Differentiating Bacterial vs. Fungal Pathology
Bacterial superinfections complicate fungal lesions through impetiginization, presenting with honey-colored crusting, rapid spread, and lymphangitic streaking. Primary fungal infections lack purulent exudate and display slower evolution. Viral exanthems typically involve vesicular patterns with prodromal symptoms, unlike the chronic scaling of fungal disease.
How to Treat Skin Fungal Infections
Topical Antifungal Protocols
First-line management utilizes topical allylamines or azoles applied to affected areas and surrounding skin. Treatment courses extend one to four weeks depending on location and severity. Terbinafine and clotrimazole demonstrate efficacy against common dermatophytes, requiring application beyond visible lesion borders to eradicate subclinical infection.
Continue topical therapy for seven to fourteen days following clinical clearance to prevent recurrence. Incomplete courses frequently result in relapse within weeks.
Systemic Intervention Criteria
Oral agents including fluconazole, itraconazole, and griseofulvin become necessary for tinea capitis, onychomycosis, or extensive body surface involvement. Dermatologists prescribe systemic therapy for immunocompromised patients or those failing topical regimens. Liver function monitoring accompanies prolonged oral antifungal courses.
Visual assessment alone cannot definitively distinguish fungal infections from eczematous dermatitis or psoriasis. Self-diagnosis risks inappropriate steroid application, which exacerbates fungal proliferation.
Bacterial superinfection requiring antibiotic therapy complicates neglected fungal lesions. Pustules, increasing erythema, or systemic symptoms indicate medical evaluation necessity.
How Skin Fungal Infections Progress Over Time
- — Microscopic fungal invasion triggers mild erythema and subclinical pruritus. Patients often mistake early symptoms for dry skin or irritation.
- — Distinctive scaling develops; ringworm lesions establish raised borders. Athlete’s foot shows interdigital maceration and odor onset.
- — Untreated lesions expand centrifugally. Concentric rings form as infection spreads outward from initial inoculation site.
- — Persistent inflammation leads to lichenification and hyperpigmentation. Secondary bacterial colonization becomes increasingly likely.
- — Long-standing infections may cause permanent pigmentary changes. Onychomycosis produces dystrophic nail thickening and crumbling.
Established Facts vs. Diagnostic Uncertainties
Confirmed Evidence
- Dermatophytes require keratinized tissue for survival
- KOH preparation identifies hyphae with high specificity
- Allylamines outperform azoles for tinea pedis
- Moisture occlusion accelerates fungal proliferation
Remaining Questions
- Genetic determinants of individual susceptibility
- Long-term ecological impacts of widespread antifungal use
- Precise mechanisms of recurrent candidiasis in immunocompetent hosts
The Environmental and Biological Context
Fungal pathogenesis requires simultaneous presence of virulent organisms and permissive host factors. Occlusive clothing, hyperhidrosis, and ambient humidity above 60% create optimal growth conditions. Community transmission frequently occurs in communal showers, swimming facilities, and locker rooms where bare feet contact contaminated surfaces.
Immunocompromised states—including diabetes mellitus, corticosteroid therapy, and HIV infection—predispose to severe, atypical presentations. Visual databases document extensive cutaneous involvement in patients with defective cell-mediated immunity.
Zoophilic transmission occurs through contact with infected companion animals, particularly kittens and puppies carrying Microsporum canis. Geographical prevalence varies, with tinea imbricata endemic in Pacific Island regions and South America.
What Medical Authorities Confirm
“Ringworm presents as red, circular, flat sores with scaly, raised outer edges. The center often clears, resembling a ring.”
— WebMD Clinical Review
“Doctors scrape the skin for microscope or culture confirmation. Visual identification alone is insufficient for definitive diagnosis.”
— Yale New Haven Health System
“Candida infections show satellite pustules around a red center, distinguishing them from dermatophyte infections.”
— Cleveland Clinic Dermatology
Summary
Accurate identification of skin fungal infections requires correlation of visual patterns—annular scaling, interdigital maceration, or satellite pustules—with clinical history and confirmatory testing. While topical antifungals resolve most superficial infections, persistent or extensive disease mandates dermatological evaluation. Early intervention prevents transmission and avoids complications including bacterial superinfection and chronic pigmentary changes.
Frequently Asked Questions
Can skin fungal infections spread to other people?
Yes. Dermatophytes transmit through direct contact with lesions, shared towels, or contaminated surfaces. Infected pets also serve as reservoirs. Household members frequently develop synchronous infections.
What causes fungal skin rashes to develop?
Pathogenic fungi colonize keratinized tissue in warm, moist environments. Risk factors include occlusive footwear, excessive sweating, compromised immunity, and contact with infected animals or humans.
How do bacterial and fungal skin infections differ?
Bacterial infections typically present with purulent exudate, rapid onset, and warmth. Fungal infections show scaling, slower progression, and well-demarcated borders without pus formation.
Are these infections more common in specific climates?
Tropical and humid subtropical regions show higher incidence due to persistent moisture. However, tinea pedis occurs globally, particularly among athletes and pool users regardless of climate.
When should I see a doctor immediately?
Seek medical care for facial involvement, widespread body distribution, nail changes, diabetes, immunocompromise, or lack of improvement after two weeks of appropriate topical therapy.
Can I exercise while treating a fungal infection?
Moderate exercise remains possible, but keep affected areas dry. Change sweaty clothing immediately post-workout. Avoid swimming pools to prevent transmission until lesions resolve completely.
Do fungal infections resolve without treatment?
Some superficial infections may self-limit, but most persist without antifungal therapy. Untreated tinea often expands and becomes chronic, while candidiasis fluctuates with environmental moisture.








